Medical researchers have successfully raised prematurely born lambs using a liquid-filled plastic pouch as a prototype artificial womb, prompting hopes the technology could one day be used on critically premature babies.The trials, carried out by a research team at the Children’s Hospital of Philadelphia, grew the lambs in a transparent pouch they called a Biobag, which allowed them to breathe lab-made amniotic fluid and continue to develop as they would in the womb.The researchers say they hope the technology might prove a breakthrough in improving the prospects for critically premature babies, who face a fight for survival even with heavy medical intervention, and often face serious health complications if they make it.“Our system could prevent the severe morbidity suffered by extremely premature infants by potentially offering a medical technology that does not currently exist,” said study leader Alan Flake, a foetal surgeon at the Children’s Hospital of Philadelphia.Fetal lungs are designed to function in fluid. By closely replicating the womb environment, the researchers hope they can create an environment to allow babies born as early as at 23 weeks of gestation to continue developing as they would until 28 weeks, when the medical risks become less severe.“If we can develop an extra-uterine system to support growth and organ maturation for only a few weeks, we can dramatically improve outcomes for extremely premature babies,” said Flake.The earlier a baby is born, the higher its risk of death or serious disability. About one in 10 babies in the U.S. are born premature – earlier than 37 weeks of gestation, rather than the full 40 – and about 6 percent are born extremely premature.Advances in technology have pushed back the limit of viability to about 23 weeks, at which point a baby has a 30 to 50 percent chance of survival, and a serious risk of major health complications, including chronic lung disease or other complications of organ immaturity.For their study, the findings of which were published in Nature Communications Tuesday, the researchers trialled the technology on lambs delivered by caesarean section at a period of gestation equivalent to 23 or 24 weeks in a human. Lambs are often used in experiments for prenatal treatment, due to the similarities with human lung development.In testing of the most recent prototype, the lambs were kept in the bags for up to four weeks. The system uses no external pump or ventilator, which could overload a baby’s underdeveloped organs; instead, the baby’s heart pumps blood through the umbilical cord into a low-resistance external oxygenator, which acts in place of a placenta in swapping out oxygen and carbon dioxide.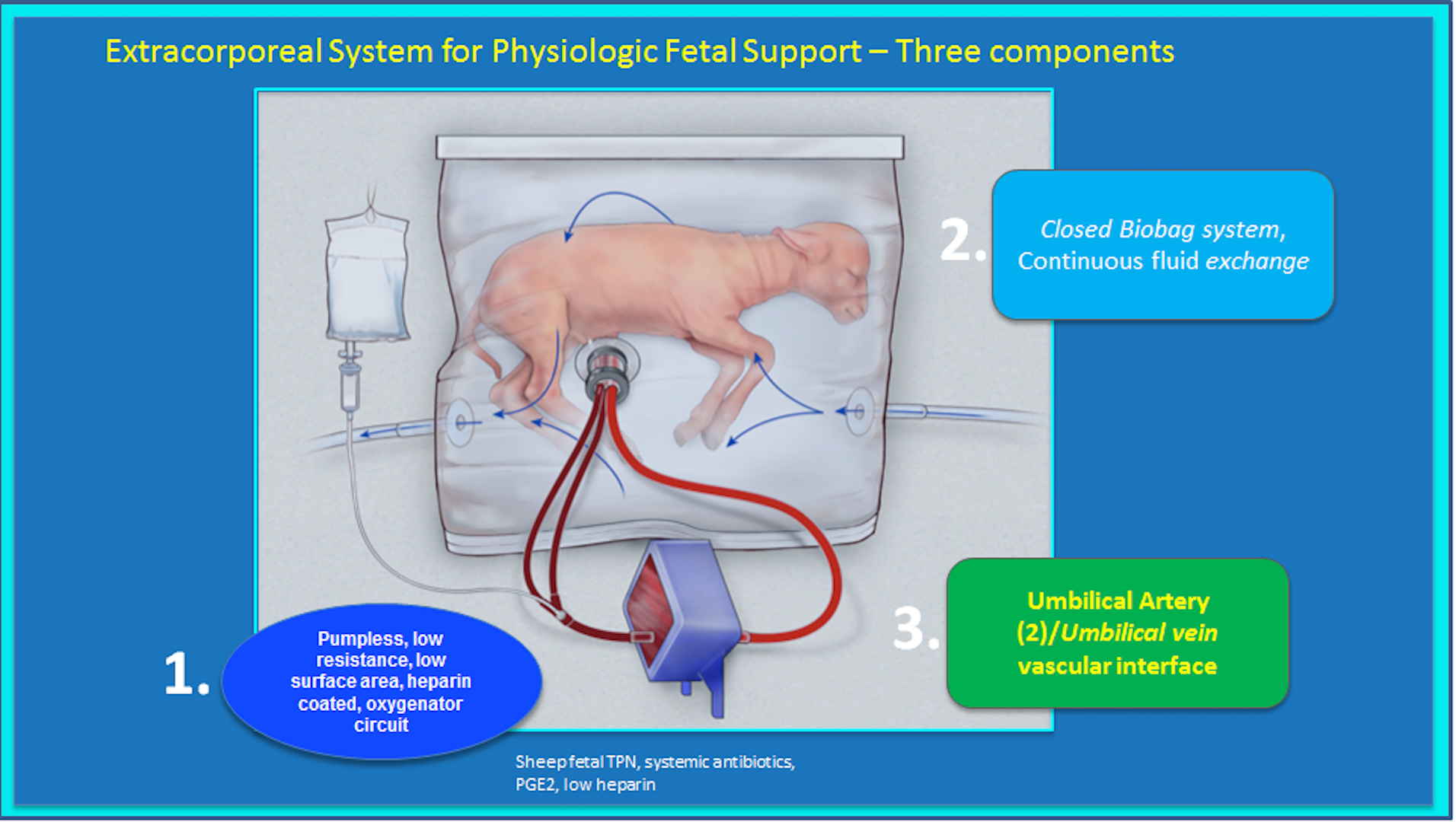 While in the sacs, the lambs exhibited normal development, growing fleece, breathing, swallowing and opening their eyes as they would in the womb. Most were euthanized so their organs could be examined, but the oldest, more than a year old, is alive and showing signs of normal development.More animal testing is required before the technology can be cleared for trial on humans, but the researchers say they hope the first clinical trials could be carried out in a few years. Flake said that he hopes that in a decade, premature babies born at between 23 to 28 weeks gestation could be raised in artificial wombs. The research team says the technology is not aimed at replacing the first half of pregnancy.Colin Duncan, a professor of reproductive medicine and science at the University of Edinburgh who was not involved in the research, told VICE News that the study was a “really attractive concept and this study is a very important step forward.”“One day this technique is likely to be part of the options for the management of extreme prematurity,” he said.But he cautioned that there were “still huge challenges to refine the technique, to make good results more consistent and eventually to compare outcomes with current neonatal intensive care strategies.”“This will require is a lot of additional preclinical research and development and this treatment will not enter the clinic anytime soon,” he said.
While in the sacs, the lambs exhibited normal development, growing fleece, breathing, swallowing and opening their eyes as they would in the womb. Most were euthanized so their organs could be examined, but the oldest, more than a year old, is alive and showing signs of normal development.More animal testing is required before the technology can be cleared for trial on humans, but the researchers say they hope the first clinical trials could be carried out in a few years. Flake said that he hopes that in a decade, premature babies born at between 23 to 28 weeks gestation could be raised in artificial wombs. The research team says the technology is not aimed at replacing the first half of pregnancy.Colin Duncan, a professor of reproductive medicine and science at the University of Edinburgh who was not involved in the research, told VICE News that the study was a “really attractive concept and this study is a very important step forward.”“One day this technique is likely to be part of the options for the management of extreme prematurity,” he said.But he cautioned that there were “still huge challenges to refine the technique, to make good results more consistent and eventually to compare outcomes with current neonatal intensive care strategies.”“This will require is a lot of additional preclinical research and development and this treatment will not enter the clinic anytime soon,” he said.
Advertisement
Advertisement
