Drug-related deaths have surged in recent years amid America’s opioid epidemic, but a new study of U.S. mortality rates suggests the problem is even worse than previously thought due to widespread misreporting of cause of death by doctors.Deaths caused by drugs, alcohol, and mental illness increased by nearly 200 percent over the last three decades, and 127 counties experienced massive spikes of 1,000 percent or more, according to research published this month in the medical journal JAMA. The authors of the study developed a way to more accurately track drug-related deaths, which are sometimes misclassified on death certificates.“It’s staggering,” said Dr. Abraham Flaxman, a co-author of the study and an assistant professor of global health at the University of Washington’s Institute for Health Metrics and Evaluation. “It doesn’t even sound right: 1,000 percent — that’s a tenfold increase.”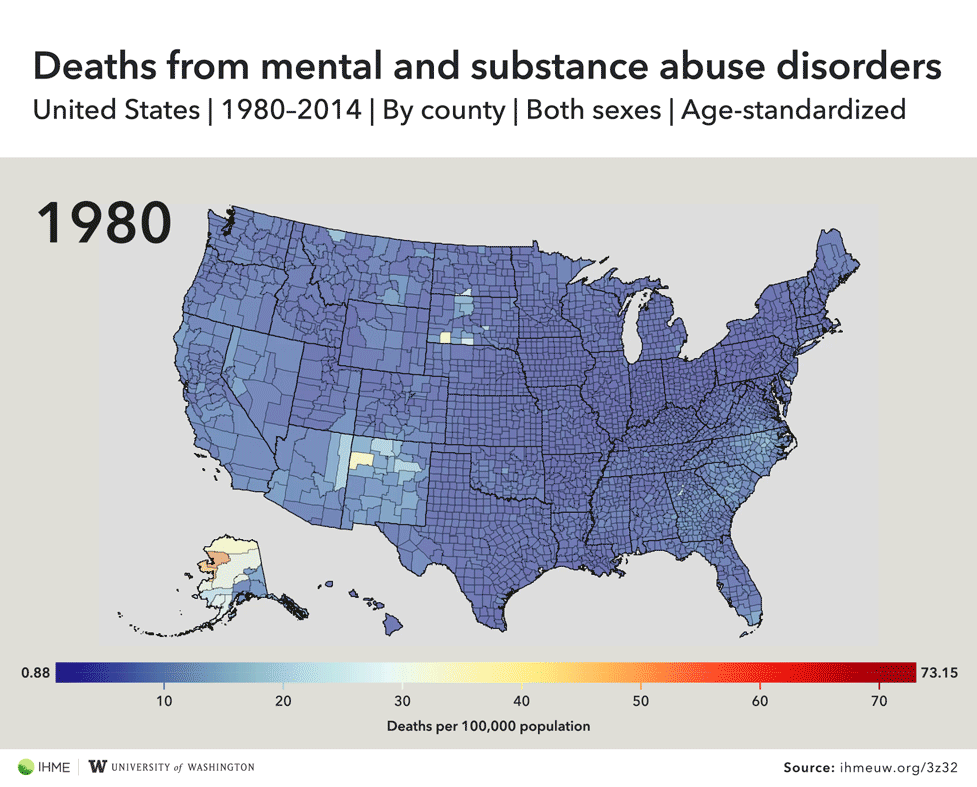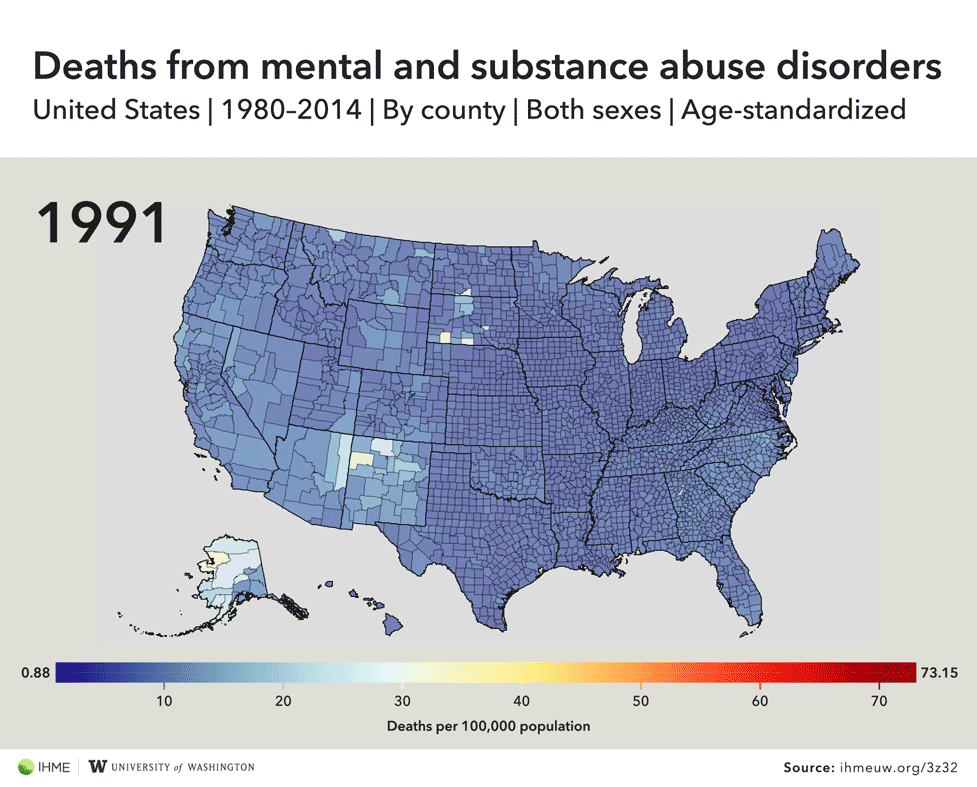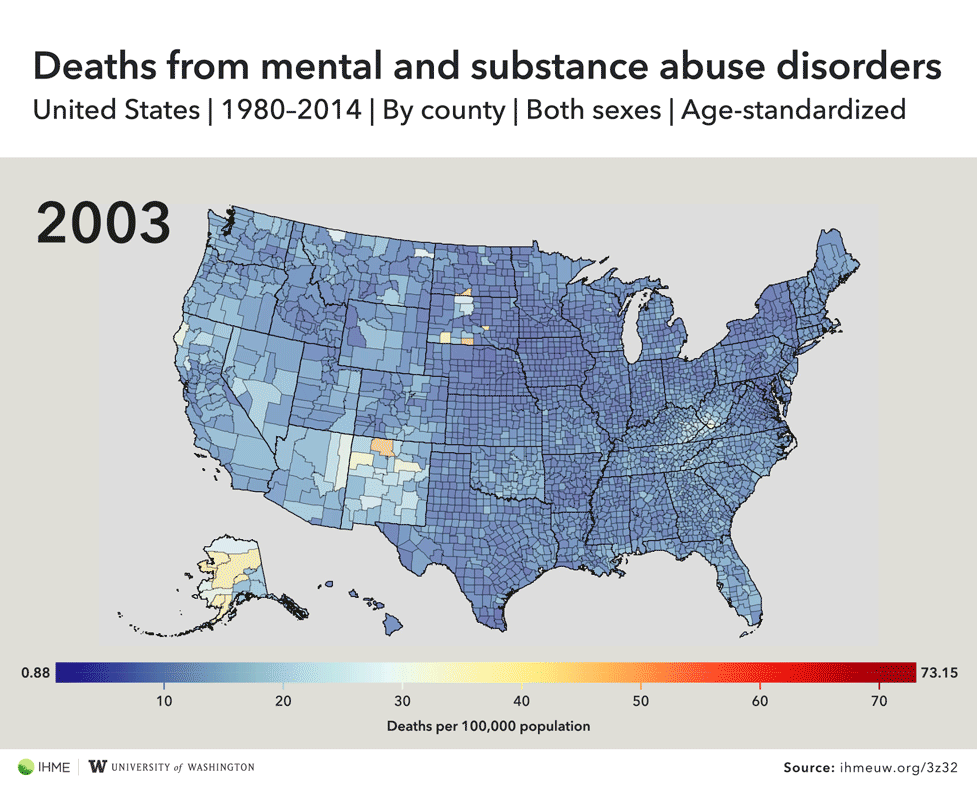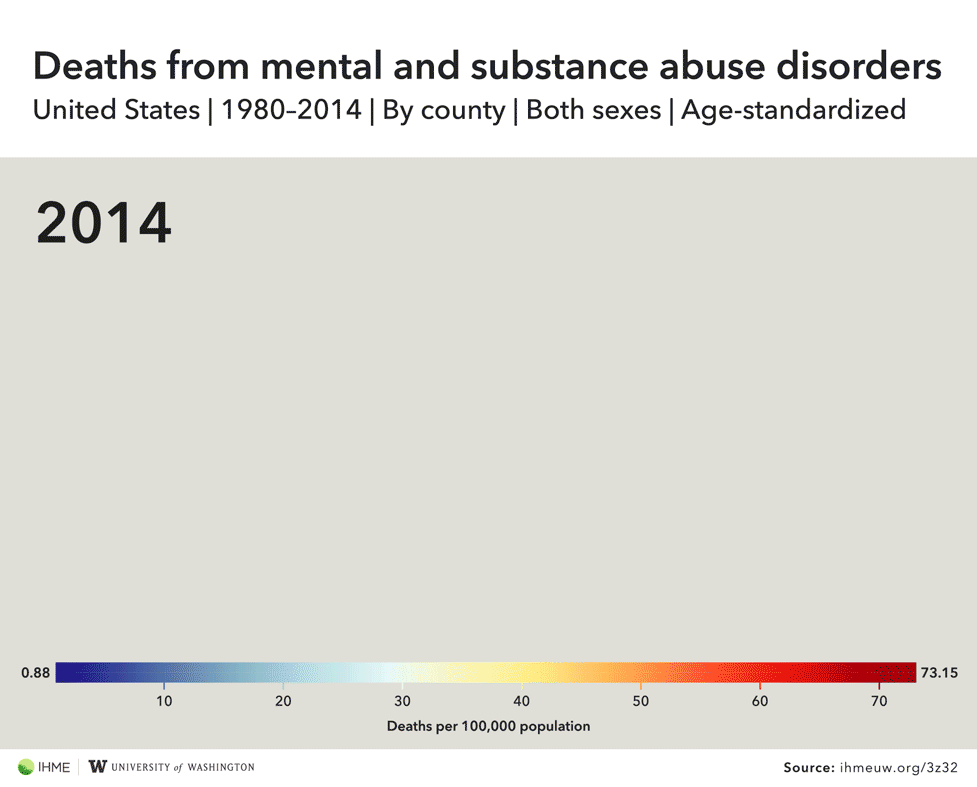 Official data from the CDC has already shown that the rate of deaths from drug overdoses increased by 137 percent across the U.S. from 2000 to 2014, and deaths specifically linked to opioids shot up again last year, surpassing 33,000.But according to Flaxman’s research, the actual death rates are much higher than the CDC numbers indicate. The underreporting, he says, is the result of doctors not accurately specifying causes of death on the paperwork they’re required to fill out when people die.Doctors typically list what killed a person on their death certificate, but it’s not as easy for them as checking a box. They must choose from more than 68,000 codes that correspond to various causes of death, a system called the International Classification of Disease. And when physicians are rushed or unfamiliar with their patients, they might choose the wrong code or one that’s not specific enough.Flaxman gave the example of a doctor who works in the emergency room. “He’s very busy, he has a lot of patients who are not dead he could be spending time with,” the researcher said. “He has somebody who just died, he maybe didn’t spend a lot of time with this person. He has to quickly figure out what to write on this form so he can go on to whatever he has to do next.”To improve the accuracy of the death certificate data, Flaxman and his colleagues “reassigned deaths with nonspecific causes to their likely underlying causes,” then developed an algorithm that was applied it to every recorded death dating back to 1980. The researchers found that deaths caused by mental and substance use disorders increased by 188 percent across the U.S., but some counties were completely off the charts.Clermont County, Ohio, an area just east of Cincinnati, saw its mortality rate from substance use and mental illness climb by 2,205 percent, according to the research. Two counties in West Virginia experienced increases of more than 2,000 percent, and the state had 16 counties with increases of 1,000 percent or more.All of the counties with increases of 1,000-plus percent were concentrated in 11 states, mostly in the Midwest and the South. Kentucky had 35 counties on the list, while Ohio had 30, Indiana had 15, and Pennsylvania had 13.Those areas have been hit especially hard by the opioid epidemic over the past decade, but Flaxman said more research is needed to confirm that heroin, fentanyl, and other similar drugs were indeed the driving factor behind the massive mortality rate surges.“The thing that is frustrating about all of this work is it says what’s going on and not why,” Flaxman said. “How people get health care has got be part of the reason why we’re seeing all of these patterns, but unfortunately we’re just scratching the surface of what’s going on.”
Official data from the CDC has already shown that the rate of deaths from drug overdoses increased by 137 percent across the U.S. from 2000 to 2014, and deaths specifically linked to opioids shot up again last year, surpassing 33,000.But according to Flaxman’s research, the actual death rates are much higher than the CDC numbers indicate. The underreporting, he says, is the result of doctors not accurately specifying causes of death on the paperwork they’re required to fill out when people die.Doctors typically list what killed a person on their death certificate, but it’s not as easy for them as checking a box. They must choose from more than 68,000 codes that correspond to various causes of death, a system called the International Classification of Disease. And when physicians are rushed or unfamiliar with their patients, they might choose the wrong code or one that’s not specific enough.Flaxman gave the example of a doctor who works in the emergency room. “He’s very busy, he has a lot of patients who are not dead he could be spending time with,” the researcher said. “He has somebody who just died, he maybe didn’t spend a lot of time with this person. He has to quickly figure out what to write on this form so he can go on to whatever he has to do next.”To improve the accuracy of the death certificate data, Flaxman and his colleagues “reassigned deaths with nonspecific causes to their likely underlying causes,” then developed an algorithm that was applied it to every recorded death dating back to 1980. The researchers found that deaths caused by mental and substance use disorders increased by 188 percent across the U.S., but some counties were completely off the charts.Clermont County, Ohio, an area just east of Cincinnati, saw its mortality rate from substance use and mental illness climb by 2,205 percent, according to the research. Two counties in West Virginia experienced increases of more than 2,000 percent, and the state had 16 counties with increases of 1,000 percent or more.All of the counties with increases of 1,000-plus percent were concentrated in 11 states, mostly in the Midwest and the South. Kentucky had 35 counties on the list, while Ohio had 30, Indiana had 15, and Pennsylvania had 13.Those areas have been hit especially hard by the opioid epidemic over the past decade, but Flaxman said more research is needed to confirm that heroin, fentanyl, and other similar drugs were indeed the driving factor behind the massive mortality rate surges.“The thing that is frustrating about all of this work is it says what’s going on and not why,” Flaxman said. “How people get health care has got be part of the reason why we’re seeing all of these patterns, but unfortunately we’re just scratching the surface of what’s going on.”
Advertisement

Advertisement